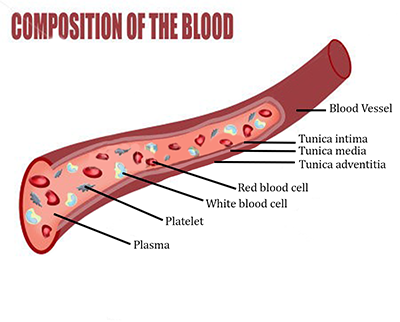
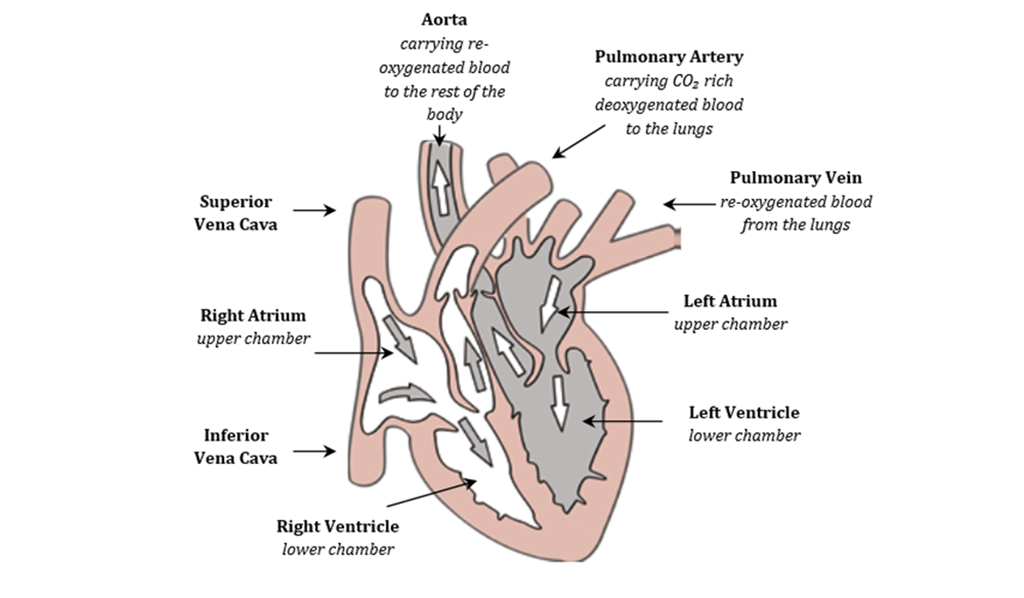
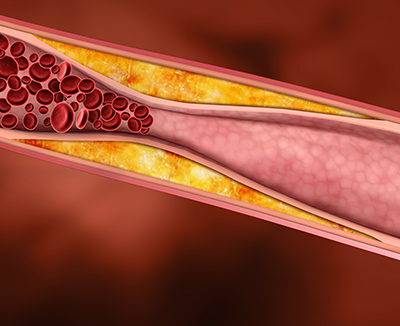
Blood vessels provide the means for blood to be transported from our hearts to the tissues of our bodies and back. Blood circulation is a continuous loop. Blood vessels are divided into different categories depending on shape and function: one type of blood vessel will gradually split or link to form another type of vessel.
Our Body is a Vessel in which we Experience Life
Circulatory System Vessels
Arteries → Arterioles → Capillaries → Venules → Veins → Vena Cava
They differ in size depending on function and position in our body. Blood vessels are responsible for transporting blood to and from our heart, therefore receiving nutrients to and from tissues.
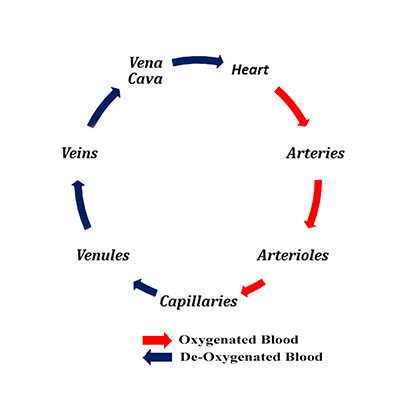
Arteries
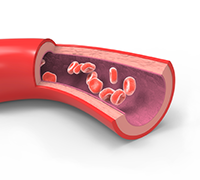
Arteries commence blood’s journey away from our hearts. Arteries have thicker muscular walls with a greater number of elastic fibres that contract to squeeze blood along passage ways away from our hearts.
Arterioles
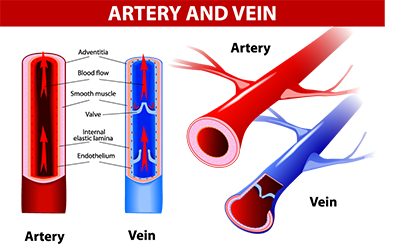
The aorta is the large artery leaving the left ventricle of the heart, dividing and sub dividing to become arterioles. The muscular walls of arteries and arterioles are thicker and more powerful than the muscular walls of veins. The main purpose of arterioles is to supply blood to capillaries.
Capillaries
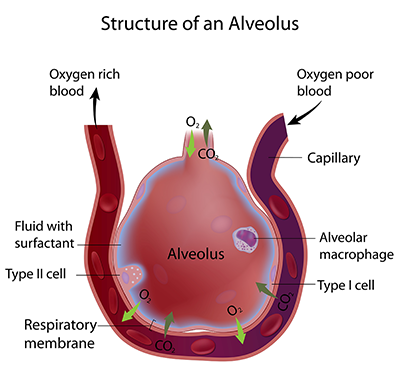
Arterioles become capillaries that spread to all parts of our bodies and have the thinnest walls, only one cell thick to allow diffusion of nutrients and gases into tissues and cells. Nutrients and oxygen pass through the walls from our blood into individual tissue cells. Likewise waste products such as CO₂ and lactic acid pass back into our blood to be carried away and excreted. Blood flows slowly through the capillary beds to allow for this exchange. There are more capillaries than any other type of blood vessel.
Venules
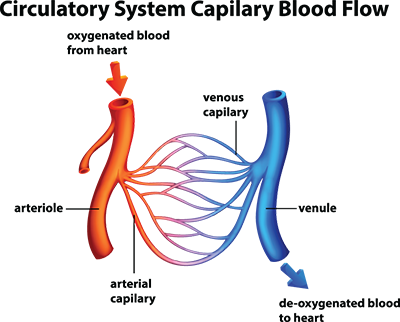
Venules begin the journey back to the heart. Capillaries pass through tissues to deposit nutrients and oxygen and pick up CO₂ and waste products; the capillaries join together to become larger vessels called venules that form larger veins carrying de-oxygenated blood back to the heart to be re-oxygenated by the lungs.
Veins
Veins have thinner walls than arteries with little contractility; they still use peristaltic action although due to low pressure a series of one way valves prevent backflow (venous return) preventing pooling in our limbs and reversed blood flow.
Vena Cava
Veins lead to the vena cava passing de-oxygenated blood from the rest of the body to the right atrium.
Summary
Veins and venules carry de-oxygenated blood high in CO₂, the exception being pulmonary veins and venules that carry oxygenated blood back to the heart.
The valves at the exit points of ventricles prevent backflow. Arteries and arterioles carry oxygenated blood around the body, the exception being pulmonary arteries and arterioles carrying de-oxygenated blood to the lungs.
Peristalsis (wave like muscular contraction) aids blood flow from the heart under high pressure. As arterial walls stretch passively they immediately contract, similar to how an earthworm moves.
Venous Return
Venous return is the flow of blood back to our heart assisted by:
- Gravity
- Non Return Valves (preventing back flow)
- The Diaphragm (assisting respiration and produces a suction effect on veins below our heart)
- Right Atrium (draws blood from vena cava in vacuum effect)
- Smooth Muscle Contraction (peristalsis happens continually)
- Skeletal Muscle Contraction (veins are assisted by squeezing action of nearby muscles)
Blood circulation is a closed system where pressure varies constantly, peaking at each heartbeat contraction, falling to lowest level just before the next heartbeat.
Hypertension is when an individual has high blood pressure meaning the pressure is constantly higher at rest.
Inactivity for extended periods slows the blood flow to lower limbs resulting in blood pooling and blood clots (DVT) that can be exasperated by sitting on a hard aeroplane seat for long periods, causing reduction in blood flow to lower limbs. It is good to incorporate a pulse lowering cool down at the finish of every exercise session to reduce blood pooling in lower limbs. Refer to: ‘The Importance of Warming Up and Cooling Down’.
How Exercise Effects our Blood Pressure
Short Term

There is an increase in SBP (systolic blood pressure) with increasing levels of exertion, in contrast DBP (diastolic blood pressure) may decrease slightly due to vasodialation or may remain unchanged, except in hypertensives where it may rise as result of an impaired vasodilatory response.
Heavy resistance and isometric exercise will increase both SBP and DBP. Hypertensives are best to avoid these and holding their breath, as this increases pressure in the thoracic cavity impeding venous return known as the valsalva manoeuvre.
Long Term
Aerobic exercise using large muscle groups in rhythmical activity helps reduce blood pressure over time, being shown to decrease SBP and DBP by 10mmHg in mild and moderate hypertensives. Strength or circuit training does not lower blood pressure; although both have other benefits.
Positive Effects of Exercise on our Cardiovascular System
- Strengthening of our heart (it is a muscle)
- Larger stroke volume (heart pumps more blood per beat)
- Heart rate (bpm) reduces due to larger stroke volume (heart’s efficiency increases)
- Arteries become stronger with greater elasticity (vessels carrying oxygen rich blood)
- Improved blood cholesterol markers (healthier cholesterol levels)
- Increased number of capillaries (oxygen rich blood reaches muscles and tissues easier)
- Increased haemoglobin count in our blood (red blood cells carrying oxygen)
- Blood pressure decreases (less stress on heart and arteries)
Control of Circulatory Blood Flow
The smooth muscles in blood vessels allow vasoconstriction (narrowing) and vasodilation (widening); either more blood or less blood can flow through them enabling our body to direct blood flow to different tissues depending on where oxygen and nutrients are required, playing a part in blood pressure regulation.
When food is eaten, blood vessels of the digestive system dilate increasing blood flow whilst blood vessels of muscles vasoconstrict reducing blood flow. During exercise the opposite occurs. Food eaten too close to exercise leaves food undigested in the stomach and leads to stitches or cramps and can sometimes lead to feeling sick or vomiting.